Opioid Withdrawal Treatment in NJ: What You Need to Know
Opioid withdraw treatment NJ is available through medically supervised programs that help you safely manage withdrawal symptoms and begin lasting recovery. Here’s a quick overview of your options:
- Inpatient withdrawal management – 24/7 medical care, typically 5-7 days, for moderate to severe withdrawal
- Outpatient detox programs – Structured treatment while living at home, best for lower-risk cases
- Medication-Assisted Treatment (MAT) – FDA-approved medications like buprenorphine, methadone, or naltrexone to ease symptoms and reduce cravings
- Partial Care / Intensive Outpatient (IOP) – Step-down support after detox, 9-20+ hours of therapy per week
- Emergency Department care – Hospitals are legally required to treat opioid withdrawal under federal law
New Jersey is one of the hardest-hit states in the country when it comes to opioid addiction. Overdose deaths jumped 29.3% in a single year (2016 to 2017). Synthetic opioids like fentanyl went from causing 35 deaths to 689 deaths between 2010 and 2016. And roughly half of all drug rehab admissions in the state are for opioid addiction.
These numbers aren’t just statistics. They represent real people — neighbors, family members, friends — who needed help and didn’t always get it in time.
Withdrawal is the wall that stops many people from seeking treatment. The physical and emotional symptoms of stopping opioids can feel unbearable. But trying to push through alone is both dangerous and rarely effective. Professional treatment makes the process safer, more manageable, and far more likely to lead to lasting recovery.
This guide walks you through everything you need to know about getting opioid withdrawal treatment in New Jersey — from what to expect during detox, to the medications used, to how programs support you after withdrawal ends.
The Impact of the Opioid Epidemic in New Jersey
To understand why Opioid withdraw treatment NJ is so vital today, we have to look at the sheer scale of the crisis in our backyard. New Jersey has historically faced some of the most challenging addiction statistics in the nation. Between 2016 and 2017, the Garden State experienced the highest increase in the number of opioid overdose deaths compared to every other state in the U.S.
The landscape of addiction has shifted dramatically over the last decade. While prescription painkillers were the primary driver in the early 2000s, the surge of high-potency synthetic opioids like fentanyl has changed everything. According to CDC Overdose Data, the national death toll exceeded 92,000 in the year leading up to December 2020, a nearly 30% increase. In New Jersey, the story is told in the sharp rise of heroin-related deaths, which increased more than eight-fold between 2010 and 2016.
The public health burden is immense. Roughly 50 percent of all admissions to drug rehab centers in New Jersey are specifically for opioid addiction. This highlights a massive, ongoing need for effective withdrawal management. It isn’t just about “quitting”; it’s about surviving a state-wide emergency that affects every demographic from Sussex County to Bergen County.

The Critical Need for Medically Supervised Opioid Withdraw Treatment NJ
We often hear from people who want to try “cold turkey” at home. While we admire the grit, the reality is that unsupervised detox is incredibly risky. Opioid withdrawal is rarely fatal on its own, but the complications—such as severe dehydration from vomiting or the high risk of relapse due to intense cravings—can be life-threatening. When someone stops using, their tolerance drops almost immediately. If they relapse during a painful home detox and use their “usual” dose, it often leads to a fatal overdose.
This is why medically supervised Opioid withdraw treatment NJ is the gold standard. Beyond just safety, there is a legal framework ensuring you get the care you deserve. A Legal Action Center Report highlights that hospitals and emergency departments have affirmative obligations under federal laws.
Under the Emergency Medical Treatment and Labor Act (EMTALA), hospitals must stabilize anyone coming in with a substance use-related emergency. Furthermore, the Americans with Disabilities Act (ADA) and Title VI of the Civil Rights Act protect patients from being turned away or discriminated against because of their substance use disorder. You have a legal right to evidence-based care, which includes screening, stabilizing medication like buprenorphine, and a “warm handoff” to long-term treatment.
Before you start, it is always wise to verify your insurance coverage so you can focus entirely on your health rather than the paperwork.
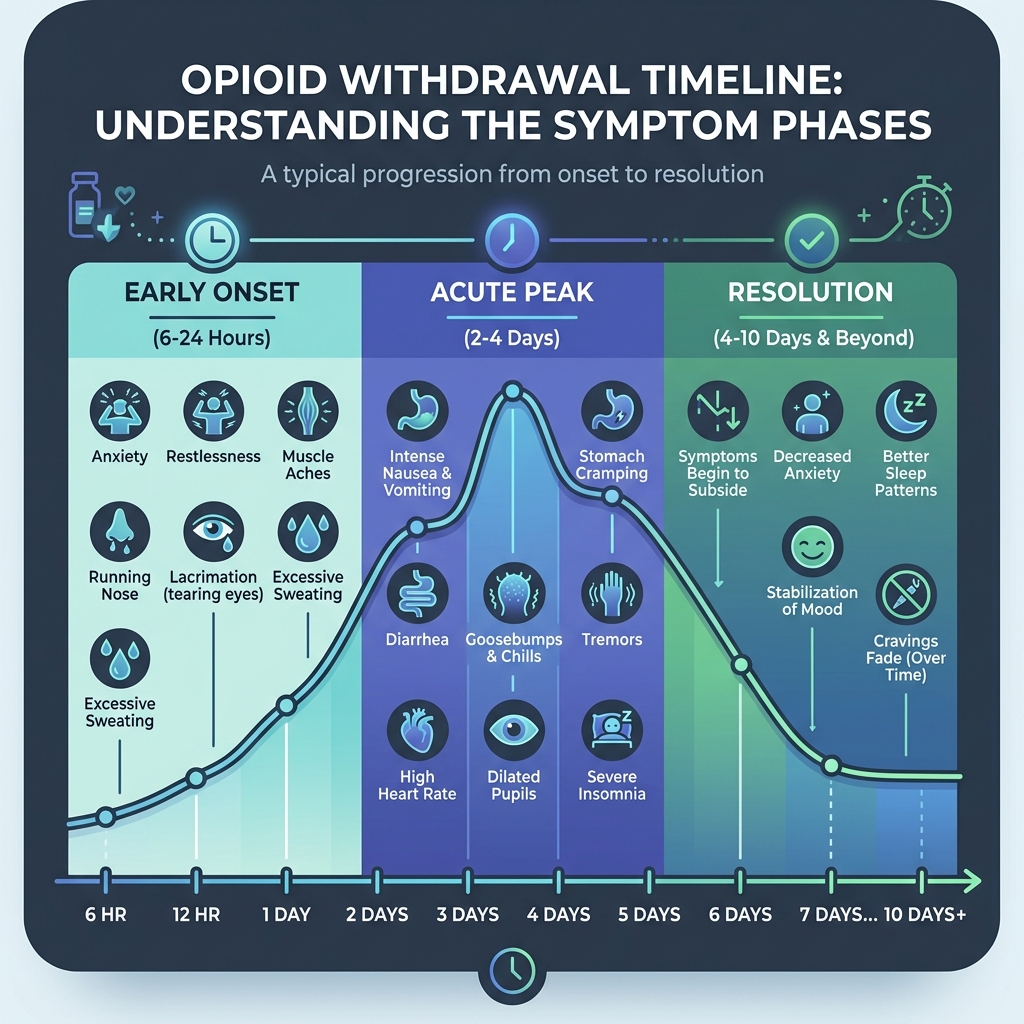
Common Symptoms Experienced During Detox
If you have ever had a severe case of the flu, you have a tiny glimpse into what opioid withdrawal feels like—but multiply that by ten. Symptoms usually begin within 6 to 12 hours for short-acting opioids (like heroin or oxycodone) and can last for a week or longer.
Common physical and emotional hurdles include:
- Gastrointestinal Distress: Nausea, vomiting, and severe diarrhea.
- Physical Pain: Intense muscle aches, bone pain, and abdominal cramping.
- Systemic Issues: Excessive sweating, chills, goosebumps, and dilated pupils.
- Cardiovascular Changes: Increased heart rate and elevated blood pressure.
- Neurological/Emotional: Severe anxiety, agitation, insomnia, and the hallmark “drug-seeking” cravings that make it so hard to quit alone.
The Neurobiology of Opioid Dependence
Why is it so hard to just stop? It isn’t a lack of willpower; it’s brain chemistry. When you use opioids long-term, they bind to receptors in the brain, specifically affecting the locus coeruleus (LC). The LC produces noradrenaline, which keeps us awake and alert. Opioids suppress this production.
To compensate, the brain ramps up its noradrenaline “machinery.” When the opioids are suddenly removed, that machinery is still running at 100 miles per hour, leading to noradrenergic hyperactivity. This “overdrive” state is what causes the racing heart, anxiety, and physical jitters of withdrawal. Understanding that this is a physical adaptation helps remove the stigma—your brain is simply trying to find a new balance.
Medications Used in Opioid Withdraw Treatment NJ
The “magic” of modern medicine is that we don’t have to let patients suffer through that noradrenergic overdrive. Scientific research has provided us with a toolkit of medications that bridge the gap between addiction and sobriety. According to a scientific review of withdrawal symptoms, effective management is the essential “gateway” to long-term success.
Key medications include:
- Alpha-2 Adrenergic Agonists: Medications like Clonidine and the FDA-approved Lofexidine (Lucemyra) specifically target the noradrenaline surge. They help reduce sweating, cramping, and heart rate without being addictive themselves.
- Buprenorphine: A “partial agonist” that fills the brain’s opioid receptors just enough to stop withdrawal and cravings but not enough to create a “high.”
- Methadone: A long-acting opioid used in highly regulated settings to stabilize patients and allow them to function normally.
- Naltrexone: An antagonist that blocks opioid receptors completely. It is often used after detox (as Vivitrol) to prevent relapse.
- Supportive “Comfort” Meds: We also use non-narcotic medications for specific symptoms, such as sleep aids for insomnia or NSAIDs for muscle aches.
The Role of Medication-Assisted Treatment (MAT)
MAT is the combination of these FDA-approved medications with behavioral therapy. It is not “replacing one drug with another.” Think of it like using insulin for diabetes. MAT stabilizes the brain’s chemistry, reduces the risk of overdose death by half, and gives the patient the mental space to engage in counseling. In New Jersey programs, MAT is considered the first-line treatment for Opioid Use Disorder (OUD) because it provides the long-term stability needed to rebuild a life.
Choosing Between Inpatient and Outpatient Opioid Withdraw Treatment NJ
Deciding where to receive care depends on your medical history, the severity of your addiction, and your home environment. You can find more info about treatment programs to see which level matches your needs.
- Inpatient Treatment: This offers 24/7 medical monitoring. It is ideal for those with high-acuity needs, co-occurring medical issues, or a home environment that isn’t conducive to recovery. A typical stay is 5-7 days, focusing on medical stabilization.
- Outpatient Detox: This allows for more flexibility. It is often called “ambulatory detox.” You visit a clinic daily for medication and check-ins but sleep at home. This is a great option for those with strong support systems and milder withdrawal risks.
What to Expect During Inpatient Withdrawal Management
When you enter an inpatient program in NJ, the first 24 hours are about assessment. You will meet with a multidisciplinary team including addiction board-certified physicians, nurses, and counselors.
- Biopsychosocial Assessment: We look at your physical health, mental health, and social situation to create a personalized plan.
- Provider Check-ins: Expect daily visits from a medical provider to adjust your medications based on your “COWS” (Clinical Opiate Withdrawal Scale) score.
- Nursing Care: Nurses monitor your vitals around the clock to ensure you are safe and as comfortable as possible.
- Therapy Access: Even during detox, you’ll have access to counselors to start processing the emotional side of addiction.
Building a Foundation for Long-Term Recovery
Detox is only the beginning. If you just do the “oil change” (detox) and don’t fix the “engine” (the underlying behaviors and triggers), relapse is highly likely. That’s why we emphasize a holistic approach.
We use Evidence-Based Practices (EBP) such as:
- Cognitive Behavioral Therapy (CBT): To help you identify and change the thought patterns that lead to drug use.
- Group Counseling: To build a community of peers who understand exactly what you are going through.
- Family Involvement: Addiction is a family disease. We help rebuild trust and teach your loved ones how to support your sobriety.
- Holistic Therapies: Yoga, art therapy, and nutrition are used to heal the whole person, not just the addiction.
Transitioning to Outpatient Care and Support
After the initial 5-7 days of withdrawal management, most patients transition to a “step-down” level of care.
- Partial Care / PHP: You spend the majority of your day in treatment but return home in the evening.
- Intensive Outpatient (IOP): 9 to 12 hours of therapy per week, allowing you to return to work or school.
- Community Resources: We connect you with local 12-step programs (like NA) or SMART Recovery groups in Sussex or Bergen County to ensure you have a “sober squad” long after you leave our doors.
Frequently Asked Questions about Opioid Detox
Is it safe to detox from opioids at home?
Generally, no. While opioid withdrawal isn’t usually fatal like alcohol withdrawal, the risk of dehydration and the incredibly high rate of relapse make home detox dangerous. Professional supervision ensures you have the medications needed to stay safe and comfortable.
How long does the opioid withdrawal process typically last?
The acute phase usually lasts 5 to 7 days. However, some people experience Post-Acute Withdrawal Syndrome (PAWS), which can include milder symptoms like sleep disturbances or mood swings that last for several weeks or months.
Does insurance cover opioid withdrawal treatment in New Jersey?
Yes. Thanks to federal and state parity laws, most insurance plans (including NJ FamilyCare/Medicaid) are required to cover addiction treatment similarly to how they cover other medical procedures. We accept most insurance plans at our facility.
Conclusion
The journey through Opioid withdraw treatment NJ is one of the hardest things you will ever do, but you don’t have to do it alone. By choosing a program that offers evidence-based medical care, compassionate support, and a holistic focus, you aren’t just getting “sober”—you are reclaiming your life.
At Woodmont Treatment Center, we provide personalized, high-end care in a luxurious New Jersey setting. We believe that everyone deserves a fresh start and the medical tools to make that start successful. Whether you are in Newton, Andover, or anywhere in the Sussex and Bergen County areas, help is just a phone call away.
If you or a loved one are ready to break free from the cycle of addiction, start the admissions process today. Recovery is possible, and it begins with a single, safe step.